Five Ways to Reduce Fall-Related Harm in Senior Living
Senior living malpractice claims
An 80-year-old resident with mild Alzheimer’s and a documented risk for falls died following a fall in the shower when a care team member left him alone to respond to an alarm in a nearby room.
An 84-year-old being bathed in the tub room with the aid of a bath chair transfer system was left alone, unbuckled, in the bath chair after a care team member left the room to find assistance to transfer the resident to her wheelchair. While the team member was gone, the resident fell to the floor, hitting her head. She later died from her head injury.
A 64-year-old resident fell from her raised bed and hit her head when the nurse left the bedside to retrieve forgotten supplies for a dressing change. She died 45 minutes later from a subdural hematoma.

Falls that result from a failure to keep residents safe are the top allegation that drives senior living claims. These fall-related harm events are typical of what was found during our analysis of Constellation senior living malpractice claims. Not only were falls the most frequent reason behind a malpractice claim, they were also the most costly.
Consistently contributing to these falls were errors in clinical judgment or poor critical thinking skills, policy not followed or absent and communication breakdowns among the care team and with the resident/family.
The top contributing factors involved in fall-related malpractice claims are:
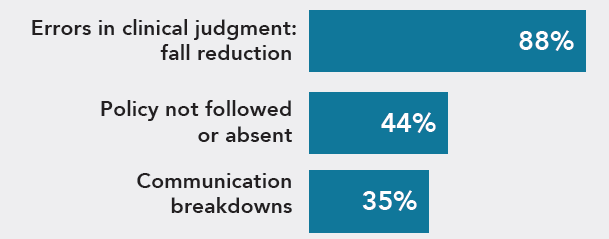
These factors contribute to harm and malpractice claims and are amenable to risk mitigation strategies. A single harm event may (and usually does) involve multiple contributing factors. A common thread in fall-related harm events was a team member leaving an at-risk resident alone to assist another resident or to seek assistance. These events happen regardless of the organization’s policy and the resident’s care plan.
Clinical judgment and critical thinking skills are used to prioritize and make key care decisions. These skills are often described as the art of applying what is learned in the classroom to actual, real-life situations. A critical thinker considers various perspectives and possible solutions when presented with a problem and then chooses the best solution for the situation. The good news? Critical thinking skills can be taught and improved upon through scenario-based learning.
“It is crucial for care team members to know how to apply critical thinking skills and receive education on methods to reduce the risk of falls during resident care situations. Investing time and resources in improving the critical thinking and communication skills in care team members creates a stronger team and can improve resident outcomes while reducing resident injury and malpractice claims.”
Monica Chadwick, Senior Risk Consultant at Constellation
In their 2020 National CBS Report, The Power to Predict, CRICO Strategies’ research shows that the odds of a malpractice claim closing with a payment to a patient/resident increase by 145% when the involved organization lacked a formal policy/protocol/program or an existing policy/protocol/program was not followed by the care team. The odds of a claim involving a fall harm event closing with a payment are 204% greater when there is a problem with a policy or protocol compared to fall-related claims without this factor.
Five ways to reduce fall-related harm in senior living:
- Assess your risk for fall-related harm events by taking our Fall Risk Assessment.
- Use scenario-based learning modules to improve team member critical thinking and communication skills related to reducing falls and fall-related injuries.
- Analyze fall harm events to determine if an issue with the fall reduction program/policy contributed to the harm. Identify if these factors were related to the absence of a comprehensive fall reduction program, the program’s purpose (we don’t need to do this) or performance issues (we couldn’t follow the program because of low staffing levels). Share lessons learned from the event analysis across your organization.
- Engage front-line team members in the development of a fall reduction program. Care team members who are involved in the fall program development and implementation have a greater understanding of the program’s purpose and feel an ownership in the implementation of the program.
- Routinely review the program for effectiveness. Track and trend fall event root causes and contributing factors to identify vulnerabilities in your fall reduction program, policies and protocols.
Policyholders can sign in to ConstellationMutual.com, navigate to the Long-term Care Bundled Solution within Risk Resources and take our Fall Risk Assessment and view resources to mitigate harm caused by falls.
The HEAL Prepare Toolkit
Our HEAL Prepare Toolkit helps your organization prepare for and respond to fall-related harm events. Unit 2, Event Response, can help you understand how contributing factors such as poor critical thinking skills, failure to follow organizational policy and breakdowns in communication contributed to the fall event.
Start your journey by taking the HEAL Assessment and then the Action Plan will guide you through the Toolkit’s four units: (1) culture, (2) event response, (3) patient communication, and (4) moving forward. Sign in to ConstellationMutual.com to access the HEAL Prepare Toolkit and HEAL Assessment found in Risk Resources.
Constellation’s HEAL program provides healing benefits for care teams and their organizations because we truly believe that what’s good for care teams is good for business.
Constellation and HEAL are trademarks of Constellation, Inc.
Share this blog article:
Latest Blog Articles
Five Steps to Reduce Generative AI Risks in Healthcare
AI is already assisting physicians and healthcare organizations in many ways. Learn how its use may impact liability and what strategies can mitigate risk.
Five Steps to Reduce Obstetrical Errors and Malpractice Claims
Learn how to reduce obstetrical harm using evidence-based protocols for managing high-risk situations, joint team fetal monitoring education, and enhanced teamwork.
How to Reduce Surgical Harm and Malpractice Claims
In an analysis of our medical professional liability claims, surgical allegations are #1 in occurrence and #2 in cost. Learn how to reduce surgical malpractice risk.
