Five Ways to Reduce Obstetrical Harm
Obstetrical harm and malpractice claims
A 26-year-old woman was admitted in the morning by her obstetrician (OB) with spontaneous contractions. He ordered Pitocin® in the evening to augment her labor. Later that night, the labor and delivery nurse paged the OB to report that the woman’s blood pressure was elevated. The OB examined the woman and ordered an epidural but did not review the electronic fetal monitoring (EFM) strip. At midnight, the nurse discontinued the Pitocin, administered oxygen and called the OB to report that the EFM strip was concerning. Despite her request that he come in to examine the woman, he dismissed her concerns, ordered discontinuation of the Pitocin and continued EFM monitoring.

Throughout the early morning hours, the nurse documented that the EFM strip showed a non-reassuring fetal heart rate pattern. At 7:30 a.m., the OB examined the woman and ruptured her membranes without reviewing the EFM strips. The OB then left to perform an elective gynecological procedure on another patient.
He returned to examine the woman at 9:25 a.m., ordered a C-section and delivered the baby at 10:32 a.m. The delivery team suctioned thick meconium from the baby and then intubated the baby due to difficult breathing. Thirty-two minutes after delivery, a neonatal transport team was called to transport the baby to a tertiary hospital NICU. A head CT was done at 23 hours of age due to persistent metabolic acidosis and poor perfusion. The CT findings were consistent with hypoxic-ischemic encephalopathy (HIE). The baby developed seizures and was started on medication.
Over the following years the child was examined and found to be neurologically impaired. The child’s parents filed a malpractice claim against the OB and the hospital alleging a delay in diagnosing/treating fetal distress resulting in permanent neurological injuries. The claim was settled with a payment to the parents on behalf of the OB and hospital. An analysis of Constellation malpractice claims reveals that OB claims are third in total cost at $107 million despite representing only 4% of all claims.
The top allegations triggering OB claims include:
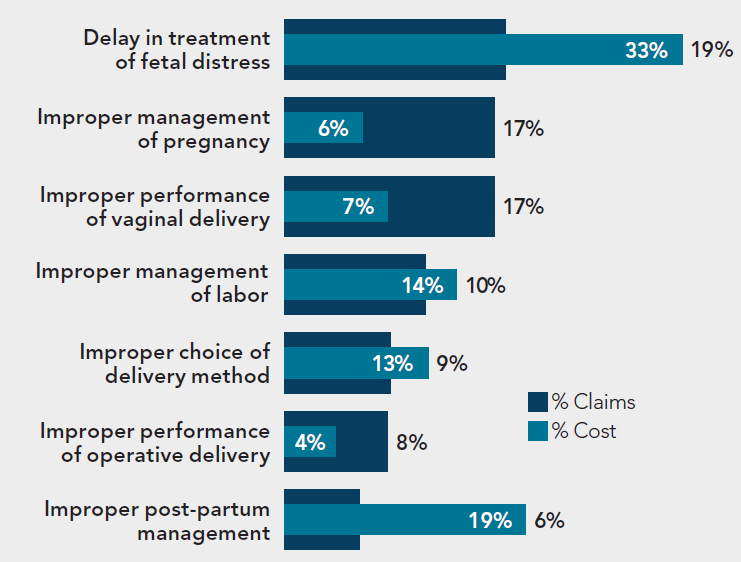
Two allegations – delay in treatment of fetal distress and improper postpartum management – represent over half (52%) of OB claim costs indicating the severity of harm involved in these events.
Clinicians and teams involved in OB claims:
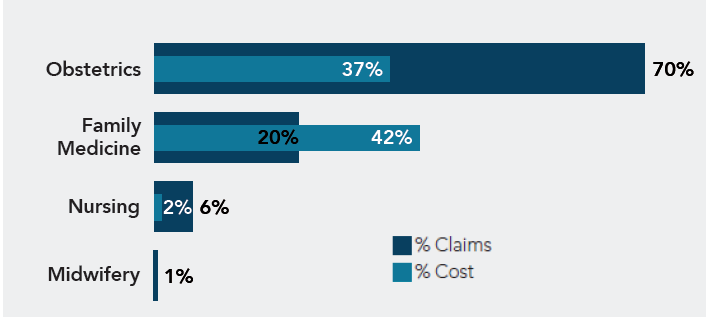
A deeper dive into OB claims reveals that 45% involve a secondary responsible clinician. Almost half of these claims involve nursing and an alleged delay in recognition and treatment of fetal distress. This is not a nursing issue in isolation but highlights a gap in team fetal monitoring and communication skills. Organizations looking to improve OB outcomes should focus on combined clinician and nursing fetal monitoring skills and team communication process education.
“Learning together as a team provides many benefits including all team members using an evidence-based process for standardized intrapartum fetal heart rate interpretation, communication and management, sharing lessons learned from past OB safety events, and boosting team morale.”
Kristi Eldredge, Senior Risk Consultant at Constellation
Five ways to reduce OB harm
- Provide joint clinician and nursing team training on fetal monitoring skills using an accredited program.
- Invest in team training and communication skills using a program such as TeamSTEPPS.
- Perform simulation drills on low-frequency, high-severity events (e.g., shoulder dystocia, OB hemorrhage, prolapsed cord).
- Implement evidence-based maternal patient safety bundles to guide practice.
- Analyze OB harm events and share lessons learned with the OB care team.
View the on-demand webinar, Contemporary Intrapartum Fetal Heart Rate Monitoring – Applying Principles of Patient Safety, and find other resources to help OB teams improve care and reduce risk: ConstellationMutual.com > Sign In > Risk Resources > Bundled Solutions > OB Risk Solutions

The HEAL Prepare Toolkit
Our HEAL Prepare Toolkit helps your organization prepare and respond to OB harm events. Unit 2, Event Response, can help you understand how contributing factors such as inadequate patient monitoring and breakdowns in team communication can affect clinician decision-making, leading to harm and causing difficulties in defending allegations of malpractice.
Start your journey by taking the HEAL Assessment and then the Action Plan will guide you through the Toolkit’s four units: (1) culture, (2) event response, (3) patient communication, and (4) moving forward. Sign in to ConstellationMutual.com to access the HEAL Prepare Toolkit and HEAL assessment found in Risk Resources.
Constellation’s HEAL program provides healing benefits for care teams and their organizations because we truly believe that what’s good for care teams is good for business.
Constellation and HEAL are trademarks of Constellation, Inc.
Share this blog article:
Latest Blog Articles
Five Steps to Reduce Generative AI Risks in Healthcare
AI is already assisting physicians and healthcare organizations in many ways. Learn how its use may impact liability and what strategies can mitigate risk.
Five Steps to Reduce Obstetrical Errors and Malpractice Claims
Learn how to reduce obstetrical harm using evidence-based protocols for managing high-risk situations, joint team fetal monitoring education, and enhanced teamwork.
How to Reduce Surgical Harm and Malpractice Claims
In an analysis of our medical professional liability claims, surgical allegations are #1 in occurrence and #2 in cost. Learn how to reduce surgical malpractice risk.
