Ten Strategies to Enhance Informed Consent
Improper informed consent leads to malpractice allegation
A 54-year-old man with complaints of diverticulitis was referred to a colorectal surgeon. The surgeon performed laparoscopic surgery to remove the diseased portion of the bowel but had to convert to an open procedure due to the amount of diseased bowel he encountered. Three days after surgery, the patient began running a fever and a CT identified an anastomotic leak. The surgeon took the patient back to the OR and placed multiple drains. The man remained hospitalized for 31 days.

Two months after discharge from the hospital, the patient began vomiting what he thought was stool. He was taken by ambulance to a tertiary center where a surgeon removed more sections of the diseased bowel and created a colostomy. One year later, he had surgery to reconnect his bowel. He was out of work and then disabled because of this complication.
The patient filed a malpractice claim against the surgeon who performed the initial surgery alleging improper performance of a procedure and inadequate informed consent. The patient and his spouse said if they had known about this potentially disabling complication they would not have consented to the procedure and instead would have opted for a more conservative antibiotic treatment first. The experts who reviewed the case were critical of the surgeon for not disclosing this known procedural risk and for failing to effectively communicate with the patient and his wife.
Understanding informed consent
Informed consent can be defined as the process by which a healthcare professional provides information to a patient about a proposed procedure or surgery, ensuring they understand the risks, benefits, complications and alternatives to treatment. This information empowers the patient to make a well-informed decision about their healthcare based on their personal values, beliefs and preferences.
Informed consent: Why it matters
Inadequate communication while obtaining a patient’s informed consent for a proposed procedure is a contributing factor in 25% of Constellation’s surgical claims. It’s also one of the more easily remedied malpractice risks that clinicians face.
Informed consent goes far beyond a signature on a consent form; it is a process of ongoing conversations that are held at critical points in the care process.
Establishing a robust informed consent policy involves input from clinicians and care team members, and a commitment to shared decision-making between clinicians and patients.
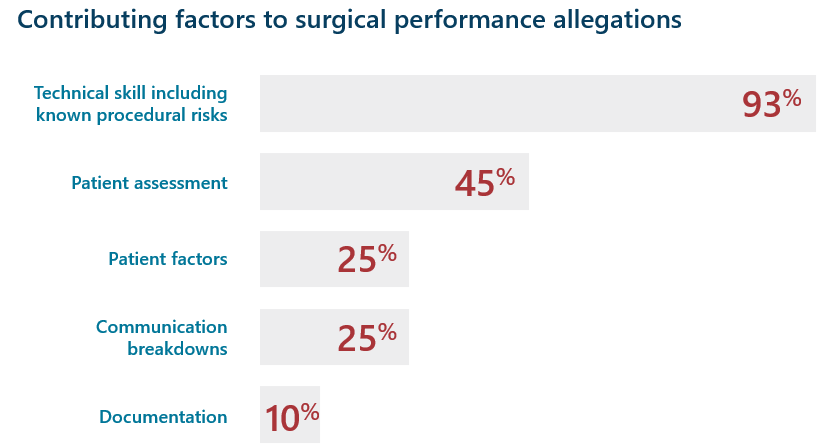
One claim can have more than one contributing factor
Constellation claims reviewed as of 12/31/2021
Vital components of informed consent
Communication and disclosure: The healthcare provider performing the medical treatment must clearly communicate relevant information about the diagnosis, prognosis, treatment options, and potential risks and benefits of the treatment, including no treatment. The communication should include any uncertainties or limitations to treatment.
Patient comprehension: It is essential for the patient to be able to understand the information provided. The provider should communicate in the patient’s primary language using layman’s terms, avoiding medical jargon, and encouraging the patient to ask questions. Visual aids such as videos, brochures or educational pamphlets can be useful tools to encourage understanding. Assessing the patient’s comprehension level allows healthcare providers to address any misconceptions or concerns more effectively.
Capacity to consent: Patients must have the mental capacity to understand the information presented, evaluate the treatment options and make an informed decision. If the patient lacks the capacity to provide informed consent due to factors such as cognitive impairment, the provider must identify an appropriate surrogate decision-maker, such as a legally authorized representative or family member.
Voluntary decision-making: Informed consent must be given voluntarily without coercion or undue influence. Patients should be allowed to accept or refuse treatment based on their personal values and beliefs, without fear of discrimination or reprisal.
Documentation: Along with the other components of informed consent, documenting the two-way conversation of informed consent is equally vital. Documentation demonstrating that the patient understood the information, was given the opportunity to ask appropriate questions, and agreed (or refused) the medical treatment is of utmost importance in aiding in the defense of a medical malpractice claim alleging improper informed consent.
Value of informed consent
- Autonomy and patient empowerment: Informed consent recognizes and respects a patient’s autonomy and right to self-determination. It empowers individuals to actively participate in their own healthcare decisions and fosters a sense of control and ownership over their wellbeing.
- Builds trust and collaboration: By involving patients in the decision-making process, informed consent strengthens the trust between patients and their healthcare providers. Open, honest communication enhances the patient-provider relationship, which leads to better collaboration and improved healthcare outcomes.
- Ethical practice: Respecting patient autonomy is a fundamental ethical principle in healthcare. By ensuring patients are adequately informed and actively participate in decision-making, healthcare providers uphold the principles of beneficence (doing good) and non-maleficence (avoiding harm).
- Risk mitigation: Informed consent plays a crucial role in reducing a patient’s perception of medical errors and adverse events. When patients are aware of potential risks and alternatives, they can make informed choices that align with their personal preferences and risk tolerance.
Ten strategies to enhance the informed consent process
Establish a robust policy to mitigate the risks involved in obtaining informed consent from a patient:
- Decide as an organization which treatments and procedures require written informed consent.
- Outline the process of obtaining informed consent from a patient, including the discussion between the treating clinician and the patient about the recommended treatment or procedure, the purpose, benefits, material risks (including known complications), possible alternatives, and the risks associated with no treatment.
- Create or obtain materials for patient education to assist in their decision-making. Consider easy to understand videos, pamphlets and online educational platforms. Instruct care team members to document any educational materials used during informed consent discussions.
- Periodically review patient educational materials to ensure they are up to date with the recommended treatment or procedural technique.
- Define the list of hierarchy decision makers who can act on the patient’s behalf based on your state laws and regulations (e.g., legal representative, next of kin, legal guardian, durable power of attorney for healthcare).
- Establish what actions to take and how to document when a patient declines a proposed treatment or procedure (also known as informed refusal).
- Delineate exceptions to obtaining informed consent (e.g., medical emergencies).
- Identify the process and necessary elements of documenting informed consent, starting with our list of recommended elements, which are detailed below.
- Consider implementing a decisional counseling program for patients and families facing difficult decisions.
- Educate clinicians and care team members on the possible legal ramifications of not obtaining informed consent, and how a quality informed consent process may provide liability protection if a harm event occurs.
*Follow: MyAccount > Risk Resources > Bundled Solutions > Surgery and Anesthesia
Share this blog article:
Latest Blog Articles
Five Steps Organizations Can Take to Reduce the Top Drivers of Patient Harm
Our national conference on reducing diagnostic, surgical, and maternal harm offered insights into the top drivers of harm. Learn how to reduce risk.
Five Steps to Reduce Generative AI Risks in Healthcare
AI is already assisting physicians and healthcare organizations in many ways. Learn how its use may impact liability and what strategies can mitigate risk.
Five Steps to Reduce Obstetrical Errors and Malpractice Claims
Learn how to reduce obstetrical harm using evidence-based protocols for managing high-risk situations, joint team fetal monitoring education, and enhanced teamwork.
