How to Reduce Surgical Harm and Malpractice Claims
Poor postoperative management leads to lifelong disability
An orthopedic surgeon performed a total knee arthroplasty on a 60-year-old man with a history of right knee pain and osteoarthritis. Six days later, on a Friday afternoon, the man called the orthopedist’s office complaining of pain and swelling in his right knee and calf. An office team member told the man to keep his orthopedic appointment the following week and to follow the postoperative instructions to use ice and elevation for swelling.
The following week, the orthopedist examined the man, who was still complaining of pain, swelling, and weakness in the right lower leg. The orthopedist ordered a duplex exam, which showed no evidence of a deep vein thrombosis. Over the next several weeks, the man continued to complain of pain, swelling, and weakness in his right lower leg, for which he called the orthopedist’s office several times.
Six weeks after surgery, the man went to his local hospital emergency department (ED) with complaints of right lower leg pain, swelling, and weakness. The ED physician ordered a Doppler ultrasound of the right knee, which showed a pseudoaneurysm of the popliteal artery, which had been injured in the initial surgery, putting pressure on the peroneal nerve. A vascular surgeon was consulted, and he repaired the pseudoaneurysm. The man suffered a permanent nerve injury and foot drop and was unable to return to work. He filed a malpractice claim against the orthopedist, alleging improper performance of surgery, failure to obtain informed consent, and improper postoperative management. After negative expert reviews, the claim was closed with a payment to the patient on behalf of the orthopedist.
Top allegations and locations in surgical claims
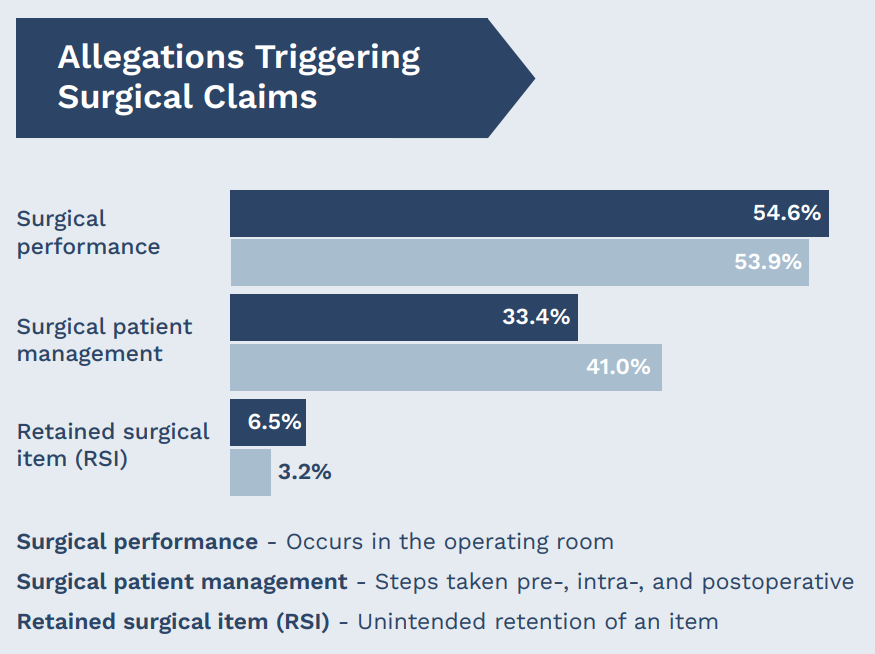
Top allegations
In an analysis of our medical professional liability (MPL) claims, surgical allegations are #1 in occurrence and #2 in cost.
Surgical performance allegations account for just over half (54%) of surgical claims and 51% of costs. In more than a third (36%) of claims, surgical patient management issues are alleged, resulting in disproportionately high costs (45%).
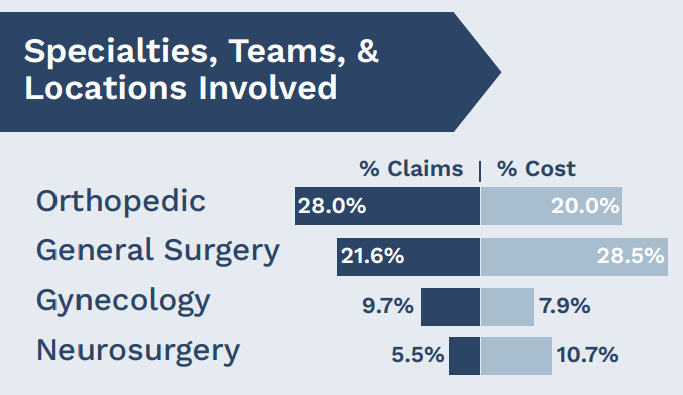
Almost half of surgical allegations involve musculoskeletal procedures, the largest group of orthopedic claims, or digestive procedures, which constitute most general surgery claims.
Top locations
Our malpractice claims analysis reveals the top locations for surgical malpractice claims:
- 46% of surgical claims occur in the OR
- 23% occur in ambulatory surgery centers
- 12% occur in medical office settings

Top contributing factors in surgical claims
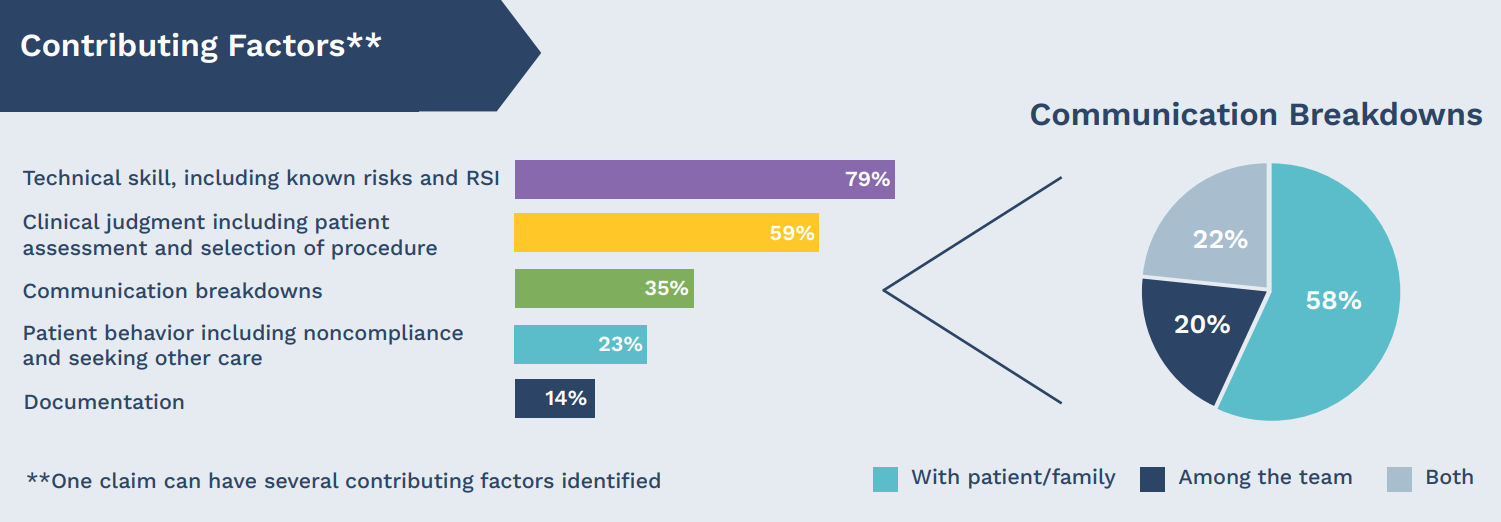
Steps to reduce surgical harm and malpractice claims
- Ensure clinician technical skill and competency with robust credentialing, privileging, and peer review processes.
- Communicate clinician privileges and scope of practice to the surgical team.
- Use a pre-op surgical risk assessment tool, intra-op checklists, documentation templates, and post-op diagnostic decision-support tools to improve the care of surgical patients.
- Employ evidence-based guidelines to manage risks, such as surgical site infections and venous thromboembolism.
- Mitigate the risk of retained surgical items by implementing count procedures/technologies and reducing distractions when setting up the operating room, during procedures, and at closing.
- Educate patients and obtain informed consent using a patient-centered, shared decision-making process that includes informed consent tools, plus a discussion of realistic expectations and post-op goals.
- Invest in team training and communication tools, especially in post-op management.
- Be transparent and communicate honestly with patients and families after a surgical harm event.
- Analyze surgical harm events using a common cause analysis tool to detect common, causal, and contributing factors and then redesign safer surgical care processes. Share lessons learned across your organization.
How to mitigate harm involved in malpractice claims
Curi and Iowa Healthcare Collaborative are coming together to offer a virtual conference highlighting the impact that harm events from the top drivers of malpractice claims—diagnostic error, surgical treatment, and obstetrical treatment—have for physicians, healthcare providers, organizations, and patients. Attendees will gain valuable insights to understand why these malpractice allegations occur, identify opportunities for improvement, and recognize how early intervention provides a better way forward for all involved after harm.
This conference will take place over three half-days on April 2, 3, and 4, 2024. Attendees will:
- Identify actionable opportunities to improve patient safety and risk mitigation
- Be inspired and learn from nationally renowned speakers who know the challenges that care teams face every day
- Gain valuable insights to understand why diagnostic, surgical, and maternal health malpractice allegations occur
- Learn how early intervention provides a better way forward after harm
There is no fee to register, and continuing education credits will be available.
Risk reports
Our risk reports analyze malpractice claim data on a wide range of topics and specialties and share insights clinicians, care teams, clinics, hospitals, and senior living organizations can use to help reduce harm events and malpractice claims. Are you a client? Sign in to MyAccount to access exclusive client versions of our risk reports. The expanded reports share actionable insights and strategies that you can utilize to help reduce harm events and malpractice claims. After you sign in, follow Risk Resources > Tools & Resources > Publications > Risk Reports. You also have access to a host of Bundled Solutions (in Risk Resources) that cover a wide variety of topics—such as Preventing Diagnostic Error—to assist you in your risk mitigation efforts.
Curi’s risk mitigation resources and guidance are offered for educational and informational purposes only. This information is not medical or legal advice, does not replace independent professional judgment, does not constitute an endorsement of any kind, should not be deemed authoritative, and does not establish a standard of care in clinical settings or in courts of law. If you need legal advice, you should consult your independent/corporate counsel. We have found that using risk mitigation efforts can reduce malpractice risk; however, we do not make any guarantees that following these risk recommendations will prevent a complaint, claim, or suit from occurring, or mitigate the outcome(s) associated with any of them.
Share this blog article:
Latest Blog Articles
Five Steps to Reduce Generative AI Risks in Healthcare
AI is already assisting physicians and healthcare organizations in many ways. Learn how its use may impact liability and what strategies can mitigate risk.
Five Steps to Reduce Obstetrical Errors and Malpractice Claims
Learn how to reduce obstetrical harm using evidence-based protocols for managing high-risk situations, joint team fetal monitoring education, and enhanced teamwork.
How to Reduce Surgical Harm and Malpractice Claims
In an analysis of our medical professional liability claims, surgical allegations are #1 in occurrence and #2 in cost. Learn how to reduce surgical malpractice risk.



