What We Learn From Obstetrical Malpractice Claims
Improper fetal monitoring and poor team communication results in an adverse outcome
An obstetrician (OB) admitted a 26-year-old pregnant woman to the hospital at 7:00 a.m. for induction. An hour after induction began, the nurse noted the baseline fetal heart rate (FHR) was 145–150, with accelerations present and contractions every 4–5 minutes. The OB ordered intermittent (every 15 minutes) electronic fetal monitoring (EFM) and that the woman could be moving about her room. Approximately thirty minutes later, the nurse noted decelerations but did not notify the OB. At 4:00 p.m., the nurse placed the woman on a birthing ball, and there were no more EFM tracings until 5:00 p.m. when the nurse noted variable decelerations.

At 6:08 p.m., the nurse noted the FHR was in the 70s and placed the woman in the bed on her left side with oxygen. She then called the OB, who arrived within 10 minutes. The OB applied a scalp electrode, noted the FHR was in the 70s with absent variability, and called in the surgical team. The team took the woman to the OR at 6:38 p.m. and delivered a baby girl by emergent C-section at 6:47 p.m.
The baby was transferred to a tertiary medical center where they diagnosed newborn respiratory distress and acidosis due to fetal bradycardia. At 5 years of age, the child has spastic cerebral palsy, is unable to speak, and walks only with assistive devices. The parents filed a malpractice claim against the OB and the hospital, alleging a delay in diagnosis and treatment of fetal distress.
Findings from Constellation’s timely care review
The experts who reviewed the care were critical of the nursing team for failing to recognize and report to the OB a non-reassuring fetal status early in the afternoon. The experts were also critical of the OB for calling for an update in the afternoon but not asking for specifics about the FHR pattern. When the review revealed problems with the care, Constellation worked with the hospital and OB to determine the best way to resolve the case. Ultimately, the claim was settled with a payment to the family on behalf of the hospital and the OB.
Top risk drivers in Constellation claims
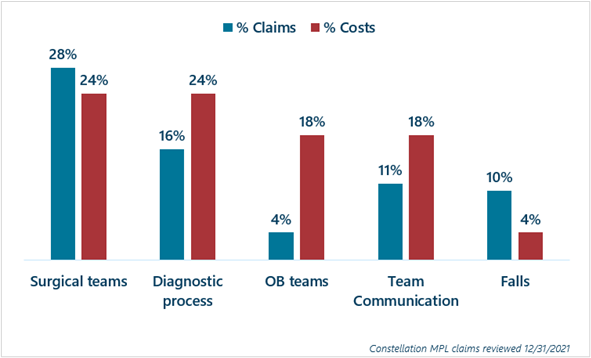
An analysis of Constellation’s malpractice claims identified the top drivers of claims and costs. OB process-related claims are third in total cost—despite representing only 4% of claims—and have the highest average settlement payments when care issues are present.
Delay in recognition and treatment of fetal distress is the top OB allegation in both percent of claims and cost.
The contributing factors involved in OB claims include improper assessment and monitoring, and team communication breakdowns. Communication breakdowns among the OB team were present in almost half (49%) of cases. The most common team communication breakdown is failure to communicate the mom and baby’s condition. A sizable percentage of these OB claims involve nursing care team members and an alleged delay in recognition and treatment of fetal distress. This highlights a gap in fetal monitoring and team communication skills.
“Recognition of non-reassuring fetal heart rate and contraction patterns, and timely communication of these issues to the OB clinician are paramount to mitigating maternal/fetal harm and malpractice claims. Clinicians must then respond appropriately when the nursing team calls for bedside examination and assessment.”
Kristi Eldredge, Constellation Sr. Risk Consultant
How to mitigate OB-related harm
A structured communication process and the right tools can improve care and mitigate OB-related harm:
- SBAR (Situation, Background, Assessment, Recommendation) is an escalation tool that provides a structured communication process nurses can use when communicating with the clinician about patient condition updates or for concerns with maternal or fetal wellbeing. The tool provides an easy to remember framework, especially in critical situations that require a clinician’s immediate attention and action.
- I-PASS handoff methodology and solutions provide a common, shared and unified structure for verbal and written hand-off communication among clinicians.
Additionally, joint clinician and OB nursing team training on EFM skills using programs like GE Healthcare’s Electronic Fetal Heart Rate Monitoring Program can also help mitigate OB-related harm. Sign in to Constellation and navigate to Risk Resources > Obstetrics Bundled Solution for an on-demand webinar and fetal monitoring education information.
The benefits of reporting harm events early
We encourage all clinicians and care teams to report unanticipated outcomes like this one early, so our team can offer our early intervention program, HEAL. At Constellation, we’re creating a better way forward after harm events—a way that can preserve relationships, promote communication and improve everyone’s experience. Our early intervention program, HEAL, champions this better way forward.
We’re prepared and ready to support our customer care teams, clinicians and health care organizations immediately following a harm event. We encourage customers to contact us as soon as possible when things don’t go as planned, so we know to offer our HEAL services.
Constellation’s HEAL program provides healing benefits for care teams and organizations because we truly believe that what’s good for care teams is good for business. To learn more about Constellation’s early intervention program, HEAL, and to assess your ability to respond effectively to a harm event like this one, sign in to Constellation to access the HEAL Prepare Toolkit and take the HEAL assessment.
Share this blog article:
Latest Blog Articles
Five Steps to Reduce Generative AI Risks in Healthcare
AI is already assisting physicians and healthcare organizations in many ways. Learn how its use may impact liability and what strategies can mitigate risk.
Five Steps to Reduce Obstetrical Errors and Malpractice Claims
Learn how to reduce obstetrical harm using evidence-based protocols for managing high-risk situations, joint team fetal monitoring education, and enhanced teamwork.
How to Reduce Surgical Harm and Malpractice Claims
In an analysis of our medical professional liability claims, surgical allegations are #1 in occurrence and #2 in cost. Learn how to reduce surgical malpractice risk.
